Life After the Knife
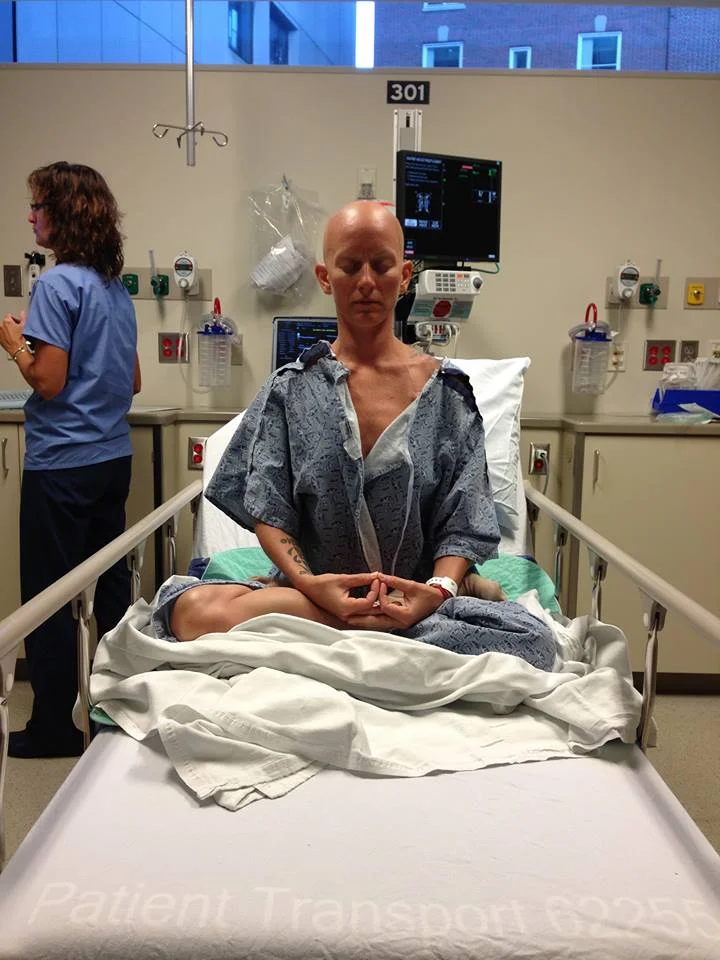
Photo by Robert Kricivich
Originally Published post-mastectomy. August 12th, 2013
Eight months doesn’t seem like a lot to exchange for the chance at living another 50 years, so I’m trying to be patient.
For me, the past 2 weeks since my mastectomy have been packed with a myriad of emotional transitions and physical alterations and it’s been tough to stay attentive. Despite my lack of physical activity, all the emotional flux I’ve been navigating has turned slow days into full days, and I find myself feeling like the last 2 weeks have both flow by and crawled along at a snail’s pace.
It’s hard to believe that 2 weeks ago I had a body of disease and today I am making big strides towards a full recovery.
According to everyone, my double mastectomy with immediate reconstruction was a great success. With the guidance of my savvy oncologist, the previous 3 months worth of chemotherapy shrank my tumor and all of it’s many calcifications and satellite spots of carcinoma to an almost undetectable presence. My breast surgeon was then able to remove all the invasive cancer from my chest, get clean margins and perform what is called a nipple and skin-sparring mastectomy.
What is a skin-sparring mastectomy, you may ask?
For those of you who are unfamiliar with this process, as I was before confronting it, this kind of mastectomy involves the removal of all of the patient’s breast tissue, but preserves a woman’s own nipple(s) and surrounding skin.
While nipple-sparring is said to alleviate some of the emotional turmoil a woman will feel following a mastectomy, sadly she will likely loose most of the sensation in her nipples. Generally speaking the pain level following this type of mastectomy is greater than that of a simple or total mastectomy, but if it were possible, I was prepared to pay that price should I be able to keep more of myself self intact.
It was originally said that I was not a candidate for this type of mastectomy given the extensive and aggressive nature of my cancer, so going into my operation, I wasn’t sure what to expect. Leading up to the operation, my team prepared me for two of possibilities: 1. single stage reconstruction with implants, or 2. tissue expanders which would help rebuild my breast over several months should everything need to be removed. I had no idea which outcome I would awake to.
Needless to say, I was scared.
I arrived at Mass General Hospital at 5:30 am with my teammates by my side. Both my partner Burr and friend Elisa helped shepherd me through not one, but two preoperative check points, and as we got closer to the surgical time of 7:00am my anxiety was mitigated only by a dose of Ativan.
The fear kicked in big time when my partner and I were greeted by my anesthesiologists who explained to me in detail the process of getting a PVB, or paravertebral block. The explanation, though sound, did nothing to make me feel better.
“PVB is an advanced nerve block technique, in which long-acting local anesthetic is injected below the muscles lateral to the spine and adjacent to the spinal nerves. Ultrasound guidance ensures correct needle placement, and the injected local anesthetic provides a band of numbness around the chest and breast area.”
Ultrasound guidance or not, I was terrified by the thought of someone sticking a needle in my back. After all, I am the girl who’s primary motivation to birth at home was to avoiding an epidural. Put another way, I’d take childbirth over a needle in my back any day.
The explanation seemed to continue on for hours. The radiologists’ voices seemed distant and distorted, as if the words came out of their mouths in slow motion. Then, all of a sudden, they disappeared. They went to check on the O.R. and the time space continuum swallowed me up. All I could hear was the thumping of my heart and the loud rush of adrenaline coursing through my veins.
Be here now, said a voice from somewhere deep inside my mind.
It occurred to me right then and there, that was exactly what I had been practicing and teaching in my yoga classes all year: being present no matter what was going on. Regardless of the mounting pre-surgical fear, this was another golden opportunity to put my money where my mouth was, and be.
Pre-op meditation. July 25rd, 2013
Be here now, the voice said again.
I fell back on my mindfulness techniques. I focused on the feel of the loose hospital garment draped over my shoulders, the sounds around me, and the cold bed beneath my seat. I remembered Thich Nhat Hahn’s gatha:
Breathing in I calm.
Breathing out I smile.
Dwelling in the present moment
It is a precious moment.
My partner was asked to clear the room and an ultrasound machine was switched on. Someone injected an intoxicating liquid mellow into my I.V. and soothing female voices began coaxing me to relax. Reflexively I started ujjayi breathing, and somehow I faded into the ether. I barely remember the nerve block going in.
The next thing I remember was thirst. Thirst, then dizziness, then nausea and then my partner. By the grace of the goddess, the marvels of modern medicine and several hundred friends and yogis praying and practicing for me around the country, my surgery was a success.
My tumor was gone.
My breast surgeon had saved my nipple, the plastic surgeon reconstructed my breasts and everything had been completed within the space of a day. As I came to my senses, I felt a tightness around my chest and a tingling in my breasts.
Breasts! Yes, I had them!
Two of them; swollen and distorted from surgery, but exactly where the old ones had been. How amazing!
I was released from the hospital two nights after my surgery. Sent home with a monstrous surgical bra and an elastic band that wrapped around my chest to keep the implants from pulling north, I felt like a walking Ace bandage. With the residual effects of anesthesia and morphine still pumping through my body I was amped-up enough to entertain company for dinner. I was alive, tumor-free
I’d love to say that things went smoothly from there on out, but I can’t. I’d love to tell you that I kept the full sense of mindfulness and presence I had found in pre-op, and that I basked continually in gratitude for my medical successes, but that wouldn't be truthful.
A knife might be less painful than depression.
The truth is, that once the last of the intravenous drugs wore off, nausea and vomiting descended upon me like locusts, eating up any excitement or enthusiasm I had had for surviving the surgery. Since I couldn’t hold food down, I weened myself off everything except Tylenol and Ativan, three days after my hospital discharge.
But once off the narcotic pain killers I was haunted by strange phantom pain in my chest and bizarre let-down reflexes in my breasts.
Every time I thought about my holding or snuggling with my son Griffin, I’d feel the hot prickling sensation of my long ago dried up milk coming in, and a floodgate of tears would stream down my cheeks. No longer having milk ducts to produce and deliver milk, nor a baby to nourish, I felt bewildered by these sensations and overwhelmed by maternal yearning.
Try Googling “phantom let-down reflex after mastectomy,” and you might get two or three hits on some breast cancer message board, and that’s about it. So little information exists out there that I thought I was just imagining things.
I made valiant attempts to stay positive, but found myself spiraling into sadness.
The dirty, dark secret thing that no one wants to talk about, the possibility the doctors don’t warn you about, the trap that Glass-Half-Full-Cancer-Warrior-Troopers aren’t supposed to succumb to, is that cancer can cause clinical depression.
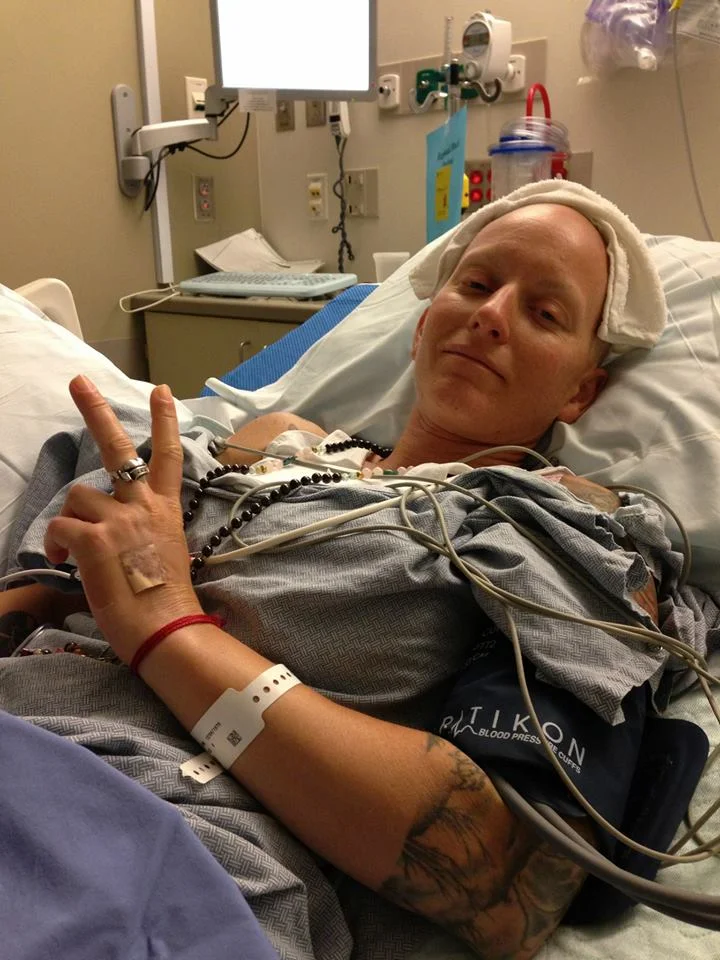
4 days post-p July 29th, 2013
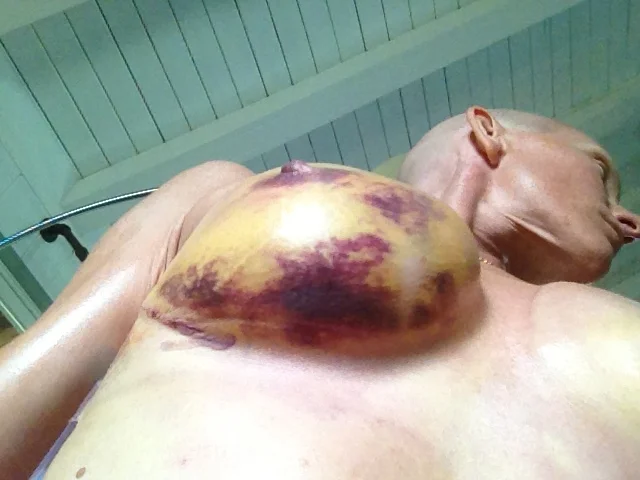
And about 7 days out of surgery, I fell into a deep, self-loathing darkness. The darkness in my heart matched perfectly the deep purple bruising spreading across my chest.
I’ve always believed that knowledge is power, so I’ve since done a little digging. It turns out that studies show as many as 1/3 of people newly diagnosed with cancer, in treatment for cancer and those who’ve survived cancer suffer from PTSD, post-traumatic stress disorder, and according to HealthNews Day, 1 in 4 women with breast cancer report symptoms of PTSD following diagnosis and/or treatment.
Symptoms of PTSD include “trouble sleeping, memory problems, irritability or anger, feelings of guilt or shame and episodes of uncontrolled sadness and crying spells” (Post-traumatic Stress via The Mayo Clinic).
Well, this explained the darkness and tumultuous tears.
I rested all of my hope on getting my surgical drains taken out as soon as possible. These drains are a package deal when you have a mastectomy and keep blood and lymphatic fluid from collecting at the surgical site. The drains are embedded inside the breast area and extend externally from your body, where they connect to collection bulbs, sometimes called grenades. The bulbs are awkward at best, and need to be fastened with safety pins to your clothes.
While the drains functionally provide an important service, they are anything but sexy (if you’re interested in more about the drains, there are hundreds of patient-made videos you can watch on YouTube), suffice to say that daily life with the tubes and drains comes with its own set of challenges.
I was crestfallen when at my July 31st follow-up appointment with my plastic surgeon, he told me I’d need to keep the drains in for at least two more weeks due to residual edema and the stubborn internal bleeding. For a short while I let this pull me down deeper into my depression.
“Let everything happen to you, beauty and terror, no feeling is final.”
~ Rainer Maria Rilke
The drains are a drag. But they are temporary! At least that’s what I keep telling myself, and isn’t that the lesson that has made itself all too clear since the beginning of this journey: that everything is temporary (beauty, youth, fertility, hair, health, even breasts). The only constant in life is change.
In her powerful and tender book, Being Well (Even When You are Sick), Elana Rosenbaum counsels those of us with illness that “To accept change, we need to accept thoughts and feelings as well as our resistance to an altered life.” I read that and thought, what sage advice.
So all that being said, I decided this week, it was time to accept my bulbous plastic friends and my depression and then maybe I would stop feeling so out of control. I've stopped fighting everything so hard and started embracing things as they are.
I took some solace in my old copy of Pema Chodron‘s seminal work When Things Fall Apart. I started walking the 1/8th of a mile to the beach a couple of times every day, and recommitted to my meditation practice. My partner came up with smart, creative ways to make the drain grenades more comfortable.We used old Kaenon sunglass bags to cover the sticky plastic bulbs (making them much less irritating to my skin) and carabiners to fasten them to my belt loops. This makes wearing the grenades more comfortable and it saves my clothes from holes made by the safety pins.
Malas: not just for mantra
Now, when I wanted to shower, we made good use of one of my many malas. It’s easy to pin the drains between the beads, and this frees up your hands for sudsing and shaving. I realized that if I ooped a long mala around my neck twice, I had enough freedom to move my arms (at least from the elbows down) to wash a good deal of my own body.
Sometimes I keep the grenades pined like this all day long. I've gotten used to looking at the fluid they collect. But If I leave the house, I cover them up. Their unsightliness could easier nauseate the unsuspecting passerby. The bulls go back in the sunglass bags and the drains get pinned back inside one of my paretner's boxy t-shirts.
If I’m teaching yoga, I wear a flowy skirt with a roll down waist band that can cover the grenades and a loose tank top on top to hide the drains. I sit on a yoga block at the front of the studio and keep pillows under my armpits to remind me from excitedly gesturing while I instruct with own my voice.
I even started going to the gym…with my parents!
As if it weren’t already sweet enough that each day this week, my father or my mother has picked me up and chauffeured me to the Nantucket Health Club, the entire staff welcomes me with open arms and showers me with encouragement. “We’re with you” they say. “You can do this!” they declare.
The reality is, I can’t do much (exercise that is); nothing with my arms until my drains are taken out, but I can ride the stationary recumbent bike. So that’s what I’ve been doing; about 10 miles a day, at a very mild pace.* The endorphins I release while exercising are giving me the kick in the ass I’ve needed to stop the depression in it’s tracks, and despite the drains, I feel better than I have in weeks.
*Patient Note: it is important not to get your heart rate up too high while recovering from surgery — exercise only under your doctor’s guidance.
My dad is a cancer survivor too. Stage IV throat cancer almost took him from us two years ago. It’s kind of a miracle he’s alive, considering he smoked well into his 50′s.
Never having been one for a workout, it’s impressive that this year he’s getting himself to a few group fitness classes per week. I’m tickled pink when we go there together: two cancer survivors, working out in the same gym, giving cancer a run for its money.
My life feels very different since I was diagnosed with cancer.
It certainly looks different. Sometimes things change at lightening speed; like the period of time from your initial diagnosis to beginning of your treatment. Other times a procedure seems to last forever: hours lost in trance watching drugs drip slowly from their IV bags. The key, I think, perhaps for all of us no matter what the struggle, is to stay present with whatever is happening, whenever possible, as much as possible and to remember each moment is temporary. One wave turns into another. Eventually, we learn to surf.
“The curious paradox is that when I accept myself just as I am, then I can change.”
~ Carl Rogers
###